




Although many books and journal articles have described that leaky gut is caused by lipopolysaccharides (LPS) in the intestines, LPS is always present in the intestines of healthy individuals and is not a direct cause of leaky gut.
For those interested in leaky gut, read the following.
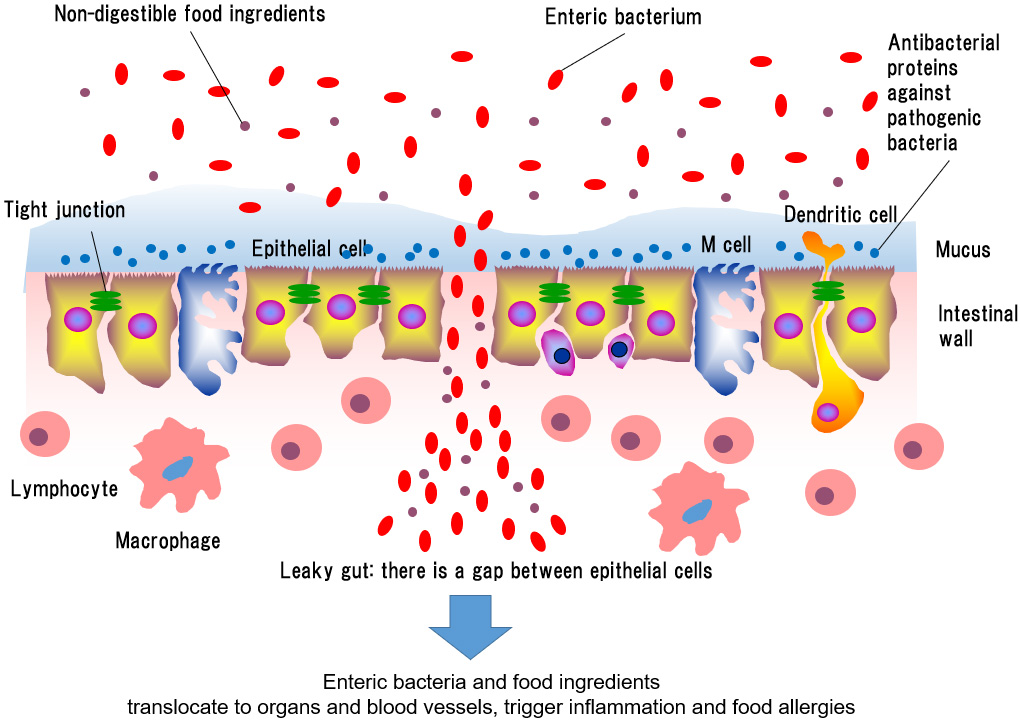
The intestines, the organ that digests food and absorbs nutrients, is where a large number of miscellaneous substances pass or stay, including food components that are not absorbed, resident bacteria, and pathogens. Thus, the intestinal wall has a special barrier system that allows absorption of nutrients while blocking substances that should not enter the body. The barrier system is physically supported by epithelial cells that make up the intestinal wall, and the spaces between the epithelial cells are tightly sealed by tight junctions (made of proteins). This barrier contains mucin-like viscous glycoproteins from epithelial cells and releases antimicrobial substances that keeps pathogens away.
Incidentally, if the tight junctions that seal epithelial cell spaces loosen for some reason, the barrier system breaks down, and what should be in the intestines slip through the epithelial cell spaces and enters the body. This phenomenon is called leaky gut.
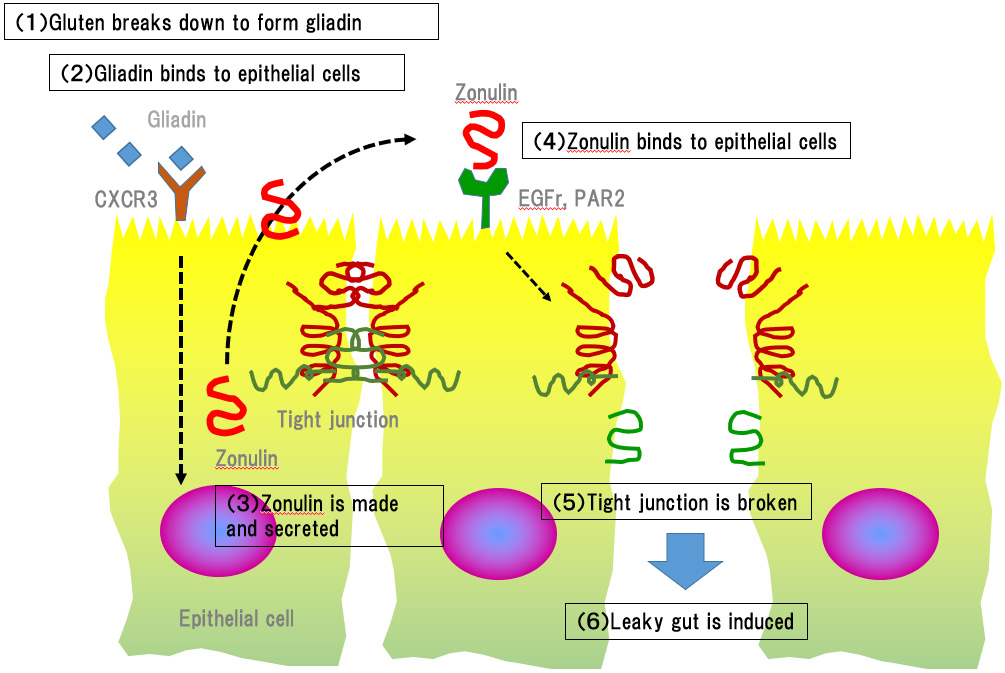
Gluten, a wheat protein, is a well-known cause of leaky gut. When gliadin, a breakdown product of gluten, binds to epithelial cells, it signals the epithelial cells to secrete a protein called zonulin excessively. Secreted zonulin binds to the epithelial cells themselves, sending a signal that unwinds the proteins that make up the tight junctions (*1, *2). In addition to gluten, alcohol (ethanol), chitosan, and capsianoside (a component in red pepper) have been reported as food ingredients that weaken tight junctions (*3). Aside from the direct effects of food, changes in enteric bacterial balance caused by stress, such as a low-fiber diet or burns, have also been reported to cause leaky gut (*4, *5).
Leaky guts allow food and bacteria to leak into the body. Food components that are harmless in the intestinal tract are recognized as foreign substances in the body and antibodies are produced, which then triggers food allergies (*1, *2). In addition, when food components and enteric bacteria, which are harmless in the intestine, migrate into the body, they are attacked by the immune system as foreign substances and inflammation occurs. If the cause is left as is without being removed, the leaky gut may become chronic and the individual may experience chronic, persistent inflammation. Chronic inflammation from leaky gut is said to promote the progression of diabetes, hyperlipidemia, obesity, and dementia.
If gram-negative bacteria enter the body, the LPS in gram-negative bacteria strongly induces inflammation. This is a well-known fact. However, LPS does not cause inflammation in the intestines, other digestive tracts, or skin of healthy individuals. Although many books and journal articles have described leaky gut as being caused by LPS in the intestines, LPS is always present in the intestines of healthy individuals and is not a direct cause of leaky gut. As mentioned above, food that passes through the intestines are considered foreign bodies and cause food allergies, if they enter the body. LPS also causes inflammation as an emergency signal when it enters the body. Oral LPS taken into the digestive tract does not need to be considered dangerous at all. Conversely, in leaky gut due to burn injuries, there has been a report that oral LPS inhibit the migration of pathogens inside the body (*6). In addition, in animal models inducing leaky gut using a drug (dextran sulfate sodium: DSS), plasma LPS levels was not elevated (*7), and rather, LPS from enteric bacteria is reported to be required for intestinal homeostasis and protection from injury (*8)
As mentioned above, leaky gut is originally caused by an unbalanced diet, such as an excess in carbohydrates (gluten) or a deficiency in fiber, or by intense stress, so it is likely to be cured by reviewing the diet to adjust the balance of bacteria in the intestines and by resolving stress.
(*1) Gliadin, zonulin and gut permeability Effects on celiac and non-celiac intestinal mucosa and intestinal cell linesScandinavian
Journal of Gastroenterology, 41: 408-419 (2006)Scandinavian Journal of Gastroenterology, 41: 408-419 (2006)
(*2) Zonulin and its regulation of intestinal barrier function:The biological door to inflammation, autoimmunity, and cancer.
Phisiol Rev. 91: 151-175 (2011) (2011)
(*3)Nutritional Keys for intestinal Barrier Modulation
Frontiers in Immunology, 6: Article 612
(*4)A dietary fiber-deprived gut microbiota degrades the colonic mucus barrier and enhances pathogen susceptibility.
Cell, 17; 167(5): 1339–1353 (2016)
(*5)Burn injury alters the intestinal microbiome and increases gut permeability and bacterial translocation
PLOS One|DOI:10,1371/journal.pone.0129996 (2015)
(*6)Commensal microflora induce host defense and decrease bacterial translocation in burn mice through toll-like receptor 4
Journal of biomedical Science, 17:48 (2010)
(*7)Inadequate clearance of translocational bacterial products in HIV-infected humanized mice.
PLoS Pathog 6(4): e1000867. doi:10.1371/journal.ppat.1000867 (2010)
(*8)Recognition of commensal microflora by toll-like receptors is required for intestinal homeostasis.
Cell, Vol. 118, 229–241, July 23 (2004)

DynaxT bldg. 2F, 2217-6
Hayashi-cho, Takamatsu-shi,
Kagawa-ken,
761-0301 Japan
TEL : +81-87-867-7712
FAX : +81-87-867-7737
Your personal information on this site is protected by SSL.